Important Benefit Info for Tobacco Users
Premiums for medical, life and critical illness insurance plans are determined partly by whether you or your covered spouse have used tobacco in the last 12 months.
Just like in previous years, there will be an additional annual premium for those who have used tobacco in the last 12 months. We do this as research shows that tobacco users are at a higher risk for health complications and chronic conditions. The additional premium helps offset their higher healthcare costs. In 2020, tobacco users enrolled in one of our medical plans will pay an additional $1,000 per person. If both employee and covered spouse use or have used tobacco, the additional premium will be $2,000. This charge will be divided by the number of Purdue pays and deducted from their paycheck.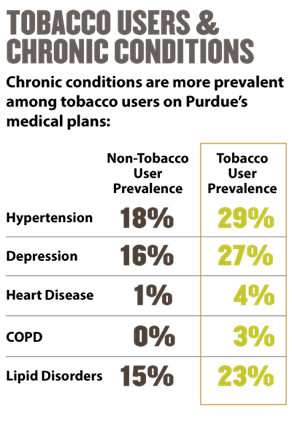
Complete Tobacco Cessation Course to Waive or Lower Premium
If you complete one of Purdue’s approved tobacco cessation courses you must turn in the certificate of completion from the program. If you have been free from tobacco for 12 months or more, you need to submit the Tobacco User Certification Form. Following a program completion or acknowledgement of 12-months tobacco free via the respective form, your premium can be lowered for all or part of the plan year.
- If you submit a form by March 31, 2020: Premium waived for the entire plan year
- If you submit a form after March 31, 2020: Premium waived for the remainder of the plan year
Sign Up for CHL Tobacco Cessation Course
Tobacco cessation courses through the Center for Healthy Living (CHL) on the West Lafayette campus are FREE and can be done either in person or via the telephone. Contact the CHL at 765-494-0111 to schedule your first session with a registered nurse health coach or pharmacist at least one week before your planned quit date.
Another Resource
Medications for quitting have been found to be effective. If you have a prescription and are covered by one of the Purdue health plans, you can receive the medication with no copay. These medications do not require prior authorization, and you’re allowed up to a 168-day supply (24 weeks) of each product in one year of treatment.