Purdue professor speaks to Congress about nanotechnology in brain treatment research
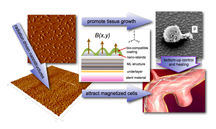
This diagram illustrates the concept behind a new type of "bioactive" coating for stents used to treat brain aneurisms, including those suffered by military personnel from head trauma due to bomb blasts. Portions of the stents - tubular structures made of a metallic mesh - will be designed using coatings to attract magnetized cells to repair blood vessels damaged in trauma. (Purdue University image/Jean Paul Allain)
WEST LAFAYETTE, Ind. — Researchers at Purdue University are working with the U.S. Army and neurosurgeons at the Walter Reed National Military Medical Center to create a new type of "bioactive" coating for stents used to treat brain aneurisms including those caused by head trauma from bomb blasts.
"Stents coated with a bioactive coating might be inserted at the site of an aneurism to help heal the inside lining of the blood vessel," said Jean Paul Allain, an associate professor of nuclear engineering. "Aneurisms are saclike bulges in blood vessels caused by weakening of artery walls. We're talking about using a regenerative approach, attracting cells to reconstruct the arterial wall."
He spoke before Congress in May during the first Brain Mapping Day to discuss the promise of nanotechnology in treating brain injury and disease.
Purdue researchers are working with Col. Rocco Armonda, Dr. Teodoro Tigno and other neurosurgeons at Walter Reed National Military Medical Center in Bethesda, Md. Collaborations also are planned with research scientists from the University of Queensland in Australia, Universidad de Antioquía and Universidad de Los Andes, both in Colombia.
Portions of the stents - tubular structures made of a metallic mesh - will be designed using bioactive coatings to attract magnetized cells to repair blood vessels damaged in trauma.
The stent coatings are modified in a Purdue facility that uses beams of charged particles called ions to modify the stent coatings with a magnetic material. The ion beams also are used to create lifelike or "biomimetic" surface textures designed to promote cellular proliferation and repair damaged vessels, Allain said.
Findings were detailed in an invited talk to be delivered by Allain during the Ninth Annual World Congress of SBMT on Brain, Spinal Cord Mapping and Image Guide Therapy on June 2-4 in Toronto.
Currently, aneurisms are treated either by performing brain surgery, opening the skull and clipping the sac, or by inserting a catheter through an artery into the brain and implanting a metallic coil into the balloon-like sac.
Both procedures risk major complications, including massive bleeding or the formation of potentially fatal blood clots.
"The survival rate is about 50/50 or worse, and those who do survive could be impaired," said Allain, who holds a courtesy appointment with materials engineering and is affiliated with the Birck Nanotechnology Center in Purdue's Discovery Park.
Cells needed to repair blood vessels are influenced by both the surface texture - features such as bumps and irregular shapes as tiny as 10 nanometers wide - as well as the surface chemistry of the stent materials.
"We are learning how to regulate cell proliferation and growth by tailoring both the function of surface chemistry and topology," Allain said. "There is correlation between surface chemistry and how cells send signals back and forth for proliferation. So the surface needs to be tailored to promote regenerative healing."
The facility being used to irradiate the stents - the Radiation Surface Science and Engineering Laboratory in Purdue's School of Nuclear Engineering - also is used for work aimed at developing linings for experimental nuclear fusion reactors for power generation.
Irradiating materials with the ion beams causes surface features to "self-organize" and also influences the surface chemistry, Allain said.
The stents are made of nonmagnetic materials, such as stainless steel and an alloy of nickel and titanium. Only a certain part of the stents is rendered magnetic to precisely direct the proliferation of cells to repair a blood vessel where it begins bulging to form the aneurism.
Researchers will study the stents using blood from pigs during the first phase in collaboration with the Walter Reed National Military Medical Center.
The stent coating's surface is "functionalized" so that it interacts properly with the blood-vessel tissue. Some of the cells are magnetic naturally, and "magnetic nanoparticles" would be injected into the bloodstream to speed tissue regeneration. Researchers also are aiming to engineer the stents so that they show up in medical imaging to reveal how the coatings hold up in the bloodstream.
The research is led by Allain and co-principal investigator Lisa Reece of the Birck Nanotechnology Center. This effort has spawned new collaborations with researchers around the world including those at Universidad de Antioquía, University of Queensland. The research also involves doctoral students Ravi Kempaiah and Emily Walker.
The work is funded with a three-year, $1.5 million grant from the U.S. Army.
Writer: Emil Venere, 765-494-4709, venere@purdue.edu
Source: Jean Paul Allain, 765 496-9718, allain@purdue.edu
