‘A challenge like no other’: Nursing alumna remembers COVID-19 vaccination work
By Tim Brouk, tbrouk@purdue.edu

Hannah Swanson, then a Purdue University Nursing senior now a 2021 alumna, applies a Band-Aid to a patient’s arm after giving her a COVID-19 vaccine shot last spring.Jayma Malme
For Kendall Landorf (NUR ’21), the 12 hours she spent working as a Purdue University School of Nursing student in two Purdue-affiliated rural health clinics where among her most memorable.
“To truly help people and help (the COVID-19 pandemic) come to an end was extremely exciting,” said Landorf, who will start her career in late July as a clinical nurse at Northwestern Memorial Hospital in downtown Chicago. “What was so cool was that it was a challenge like none other, and we had to utilize so much that was in our toolbox for what had become a very personal matter.”
Greater Lafayette needed help getting shots into arms around the community. In turn, dozens of Purdue nursing students gained valuable experience working at multiple vaccination sites, including one set up on campus in the Frances A. Córdova Recreational Sports Center.
Landorf was assigned to help with the initial heavy demand for COVID-19 vaccinations at two of the four Purdue-affiliated North Central Nursing and Family Health Clinics. She logged six hours at the Delphi clinic in White County and six more at the health center in Burlington, a Carroll County town with a population of 603.
The influx of Purdue nursing students to these rural clinics not only helped with demand but also gave them experience working for populations that are underserved and unable or unwilling to travel to larger cities like West Lafayette.
All nursing students were fully vaccinated before they picked up these shifts. Landorf started in early March and was met with an enthusiastic — and sometimes emotional — wave of patients. Most were elderly, and not all were from Carroll County or even Greater Lafayette. Landorf said she treated a woman from Carmel who drove 90 minutes to get her shot.
“It was wonderful to see how eager they were to get it,” Landorf added. “In nursing, we don’t have a lot of days that are really encouraging, but to see a lot of people get excited about something that we’ve been waiting for so long after feeling a lot of heaviness, it was a breath of fresh air.”
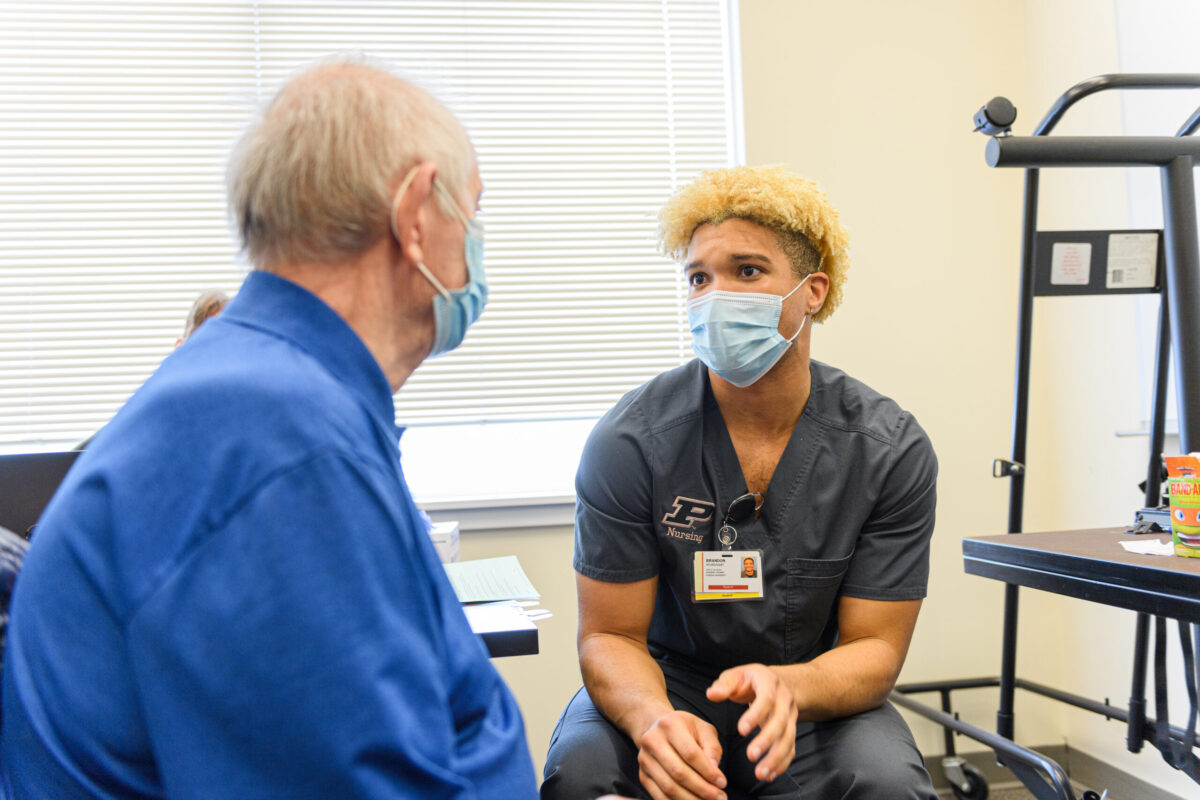
Brandon Sturdivant, then a Purdue University Nursing senior now a 2021 alumnus, discusses vital COVID-19 vaccine information with a patient last spring at a nursing clinic in Delphi.Jayma Malme
Therapeutic communication
Landorf was thrilled to be part of a historic time in healthcare. The range of emotions that came with administering doses of Moderna or Johnson & Johnson vaccines was palpable, and working with small-town patients was a new experience for the Dallas, Texas, native.
“I learned so much about Indiana — all of the little towns — from the patients,” Landorf recalled with a laugh.
Landorf dug into her therapeutic communication skills with her patients. These soft skills were introduced to her early in her classes, and being able to implement them in real-life, potentially intense situations like giving out COVID-19 vaccine shots was a thrill.
“It was a deeply personal matter for a lot of patients,” Landorf said. “It was also something new, and something new can be scary.
“They valued personal experience a lot. When I was educating patients, they really valued my personal experience with the side effects and what the data says about the vaccines. People were really attentive to what you had to say, and for me, I realized the power of a story and staying very educated in the research myself. Patients took my word as gospel.”
But the mental aspects of COVID-19 vaccination could not be left at the clinic. Landorf lived with four roommates, who were unvaccinated at the time. While everyone had to navigate such a landscape during the pandemic, Landorf and her fellow nursing seniors had a distinct perspective.
“It’s just been very complicated when you’re a nurse and you’re bringing home all of the responsibility of COVID and all of your contacts,” Landorf explained. “But you’re also a college student, so you’re living with four other roommates who go out or don’t go out or do other things.
“It’s just a large burden that you carry with you when you are a healthcare professional seeing all of these patients.”
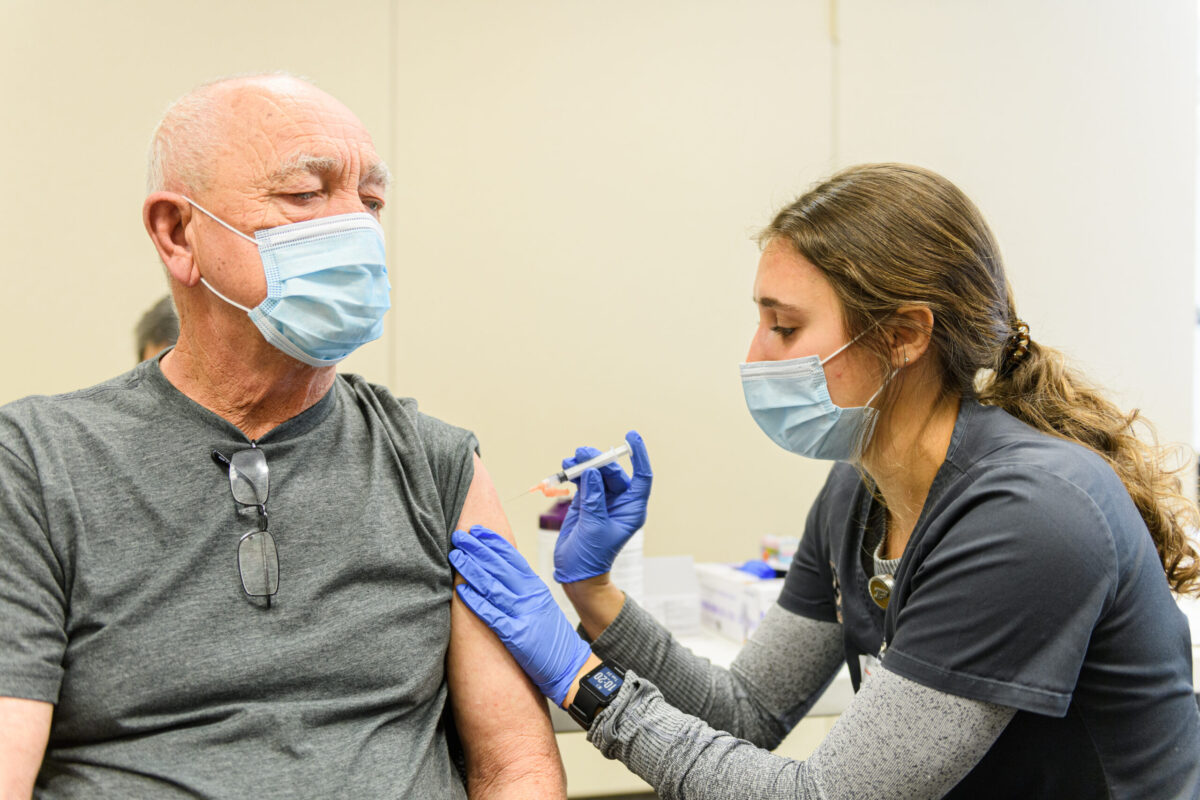
Lena Chalian, then a Purdue University Nursing senior now a 2021 alumna, gives a shot to a patient last spring at a nursing clinic in Delphi.Jayma Malme
Vaccination hesitation
Landorf used some of her therapeutic communication to calm hesitant patients. However, vaccine hesitancy was a problem in much of Indiana and other parts of the United States, especially after the first couple waves of healthcare workers, older adults and other at-risk patients were vaccinated. As younger demographics were allowed to get shots, the rates plateaued or dropped in many areas.
After she completed her shifts in Carroll and White counties in April, Landorf wanted more experience in vaccination work. She signed up to volunteer at a Riggs Community Health Center in Lafayette. However, she was told her help was not needed as demand had fallen by late April.
More sobering were the multiple healthcare workers at the clinics who said they were not going to get the vaccine. Of course, minds could have changed since March, but it proved how COVID-19 vaccines brought out strong feelings, which had to be countered with reassurance backed by strong data.
It’s now been two months since Landorf’s last shift administering COVID-19 vaccines. As of June 11, vaccination rates stood at 43.1% for the U.S. for those who are considered fully vaccinated, but only 36.7% for Indiana. Some states are better, some are worse. For those still holding out on getting vaccinated, Landorf said it’s best to listen to the science behind the shots.
“I think the best thing we can do is to be willing to get informed, to get educated,” she added. “Know really what research says and hold perspective.”
Historic learning experiences

Jennifer CoddingtonAllyson Corba
While every semester affected by the COVID-19 pandemic has had its harrowing moments, Jennifer Coddington, director of practice and outreach for the School of Nursing and the pediatric nurse practitioner program as well as medical director for North Central Nursing Clinics, revealed that the clinics reached out to Purdue Nursing for assistance just a few days before classes started in January. Students were quickly vaccinated and mobilized.
Coddington saw the opportunity to work with COVID-19 vaccines would be invaluable, from learning how the vaccines were stored and handled to getting trained on the computer system connected to COVID-19 vaccination processing. For example, Moderna vaccines had to be in a deep-freeze while Johnson & Johnson just had to be kept in a refrigerator between 36 and 46 degrees. Then came working with patients from very different backgrounds and demographics.
“Our main purpose was to serve the low-income and underserved populations,” Coddington said. “We were asked to help these patients in rural areas who have less access to care and get them vaccinated. I think our clinics became very important to reach out to those individuals that didn’t have a lot of access to getting to a pharmacy or getting to a vaccination clinic.”
More importantly, the boost Purdue nursing students gave to the rural clinics led to more vaccinations and closer steps to health normalcy. Coddington reported 8,000 shots given at the clinics during the spring semester, and the students handled many of those.
“The students were very integral in keeping things running,” Coddington said. “The undergraduate students just jumped right in. I don’t think we could have kept things running without these students.”
Discover more from News | College of Health and Human Sciences
Subscribe to get the latest posts sent to your email.