Bridging the gap between theory and clinical practice: Simulation center prepares students to navigate the complexities of health care
Written By: Kat Braz
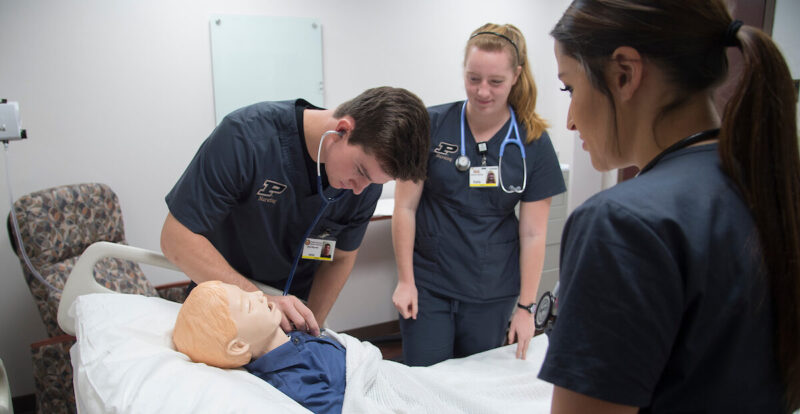
Nursing students complete a simulation in the Center for Nursing Education and Simulation.
Alarms sound and stress builds as a patient admitted for chest pain goes into cardiac arrest. The nurse calls the code, begins chest compressions and quickly explains what should happen next.
Students in the School of Nursing navigate low frequency high-risk scenarios such as this in the Center for Nursing Education and Simulation (CNES) on a routine basis. Although the patient is a high-fidelity simulator mannequin and not a live human, for the nursing students, the stakes feel just as high.
“Students take the simulations very seriously and become engaged with the patients,” said Amy Nagle, clinical assistant professor of nursing and director of simulation. “Every patient has a backstory to help give them a personality and create an emotional connection because that is the reality of practice. To be an effective health care professional, you must see patients as individuals with life experiences that shape them and family members who care for them.”
Simulation serves a critical role in bridging the gap between theory and real-world clinical practice. The simulators, which have voices, heart, lung and bowel sounds, pulses and programmable vital signs, help immerse students in realistic clinical situations. In the complex and dynamic field of health care, it is imperative for nursing students to gain practical experience and develop quality skills in a controlled, risk-free environment. The CNES allows students to make mistakes and learn from them without causing real harm.
“Students know it’s okay to make mistakes because we always debrief afterwards,” Nagle said. “Although students also participate in real-life clinical placements, they don’t often experience a situation where a patient collapses and goes into cardiac arrest. But they might encounter that in practice and we want them to feel prepared. I’ve had graduates tell me that the first time they responded to a code on the job, they felt more confident about their skills because of their experience with that simulation.”
The CNES has five individual hospital rooms, each with its own debriefing room, that can each accommodate up to eight students and one faculty member, allowing different simulations to run simultaneously. Faculty develop simulation scenarios that align with their course curricula and as director of simulation, Nagle ensures every simulation follows best practices and is appropriate for the level of the students. In addition to the 120 credits required to earn a bachelor’s degree, students must also complete 855 hours of clinical training, up to 25% of which can take place in the CNES.
“We’re very fortunate to have very good facilities in the CNES but there is no room to expand,” Nagle said. “In the new Nursing and Pharmacy Education Building, we’ll have 12 simulation rooms and the rooms themselves will be larger.”
The additional space is necessary to satisfy the growing need for simulation time and better accommodate students’ schedules. Right now, some simulations must be scheduled in the evenings. In planning for the new building, the faculty is working closely with a company that specializes in designing simulation centers to ensure the new facility will address current needs and allow for growth. The additional space also opens up opportunities for interprofessional simulation with students from pharmacy, athletic training or speech, language and hearing sciences, allowing for more cross-disciplinary collaboration.
“The Center for Nursing Education and Simulation is an essential, strategic component of Purdue’s Bachelor of Nursing program,” said Nancy Edwards, interim head of nursing. “By immersing students in lifelike scenarios that mimic the challenges they will encounter in actual patient care settings, simulation not only enhances their ability to deliver high-quality care but also cultivates a deep sense of empathy and compassion. These skills ensure that our students are well-prepared to navigate the complexities of the profession with competence and care.”
Discover more from News | College of Health and Human Sciences
Subscribe to get the latest posts sent to your email.