 Purdue News
Purdue News
 Purdue News
Purdue News
 Purdue University researchers have developed a process called fluorescence lifetime
imaging, which can be used to produce images of the biochemical makeup of the body's
tissues. It's a technique that may provide more specific information than traditional
imaging technologies such as X-rays and magnetic resonance imaging (MRI), says Eva
Sevick, associate professor of chemical engineering.
Purdue University researchers have developed a process called fluorescence lifetime
imaging, which can be used to produce images of the biochemical makeup of the body's
tissues. It's a technique that may provide more specific information than traditional
imaging technologies such as X-rays and magnetic resonance imaging (MRI), says Eva
Sevick, associate professor of chemical engineering.
"In the earliest stages of disease, certain biochemical changes take place in tissues, even before the structural alterations that can be seen under a microscope," she says. "For example, changes in the oxidation state of enzymes involved in cell respiration indicate a change in metabolism, which may mean cancer is present. X-rays and MRIs can't detect these early changes, but this fluorescence imaging might. And early detection of disease may improve its prognosis."
The process is described in a paper currently under review for publication in the journal Applied Optics . The paper was presented in March at a meeting of the Optical Society of America.
Fluorescence lifetime imaging relies on monitoring the light emitted, or fluoresced, by molecules after a harmless laser has been shined through a body part or tissue sample. Though it hasn't yet been tried on human tissue, Sevick says the technique shows great promise for detecting cancer, and could be used to determine whether a tumor is benign or malignant.
In Sevick's laboratory, research associate Dilip Paithankar spent two years determining how chemicals fluoresce and developing a computer program to generate simulated images of tissue based on fluorescence. The researchers recently filed a patent application for the program and for the use of fluorescence lifetime imaging in tissues.
Their next step will be to demonstrate the imaging technique using pet dogs that have developed breast cancer. The project, which also involves Dr. Dave Waters in Purdue's School of Veterinary Medicine, calls for optically imaging dog breast tissue in vivo before the cancerous tissue is removed and then comparing the images with the removed tissue.
"In the dog study, we hope to demonstrate the efficacy of this technique for detecting cancer," Sevick says. "Hopefully the technique will uncover diseased tissue where none has been detected through palpation." The study is funded by the National Institutes of Health.
While fluorescence imaging won't replace X-rays and MRIs, it might fill niches that other technologies can't, Sevick says. X-rays are used primarily to look at bones, teeth and other dense tissue, while MRIs look at the structure, and to a limited extent the biochemistry, of soft tissue.
"Fluorescence imaging may provide more specific biochemical information, and for most applications should be safer, faster, easier to use and less costly than other methods," Sevick says.
For example, a typical fluorescence imaging system would consist mainly of a computer, a light detector and a few small laser diodes, "the same diodes that are found in CD players and grocery store scanners and that cost less than $1 apiece," Sevick says. "Compared to MRI equipment, which costs around $3 million and another $1 million in operating costs each year, this system would be much more economical."
The technique depends on measuring the "lifetime" of molecules that have been energized when they absorb light. The lifetime is the time it takes for these molecules to relax to a ground energy state, releasing fluorescent light in the process. Lifetimes are typically a billionth or a trillionth of a second.
In the Applied Optics paper, Christina Hutchinson, a research associate in Sevick's lab, demonstrates how such lifetime measurements can be made in tissues. Because near-infrared light from a laser can penetrate through several inches of tissue, such as a breast, Paithankar has been able to adapt the technique to produce images. Here's how it works:
A detector gathers the fluorescent light and a computer program tracks the time it takes for fluorescence to occur, which is the optical relaxation time or fluorescence lifetime. Based on the lifetime, the computer program generates an image which may, for example, show the metabolic state of the tissue, indicating disease is or isn't present; or map the chemical's concentration and distribution, indicating the boundaries of diseased tissue such as a tumor.
"No one else has done this," Sevick says. "It's almost 'Star Trek'. On that TV show, the doctor has a device that emits some form of radiation, scans it over a patient and receives the signal coming back. That's not so far from reality."
In the more immediate future, Sevick says fluorescence imaging could be readily applied in a clinical setting.
"As with other conventional imaging modalities, fluorescence lifetime imaging may require a contrast agent," she says. "Consequently, a patient may first drink or be injected with a chemical tracer or drug that tends to accumulate in diseased tissue. Some of these drugs currently on the market also fluoresce. In theory, if you give an injection of fluorescent agent to someone who has a high risk for disease, such as breast cancer, one can determine the presence of the disease."
In the case of breast cancer screenings, Sevick says fluorescence imaging might be safer and less painful for patients who are genetically predisposed to getting the disease, and who often must undergo frequent x-ray screenings and biopsies of breast tissue.
"Frequent mammograms may not have as great a positive benefit as one would expect," Sevick says. "Yet women who are at high risk for the disease can't be diagnosed in the early stages if they aren't screened on a regular basis."
Sevick says women with fibrocytic disease and who are at high risk for breast cancer experience false positive mammograms approximately 80 percent of the time. Positive mammograms typically result in a needle biopsy.
"A needle biopsy of the breast can be very traumatic and expensive," Sevick says, "especially when it is unwarranted in 80 percent of the cases. I think for most women, a needle in the arm would be far less traumatic than a needle in the breast."
Sevick's work is or has been funded by the Department of Defense, the National Science Foundation, the National Institutes of Health and the Whitaker Foundation.
Source: Eva M. Sevick-Muraca, (765) 496-2377; Internet, sevick@ecn.purdue.edu
Writer: Amanda Siegfried, (765) 494-4709; nternet, amanda_siegfried@purdue.edu
Purdue News Service: (765) 494-2096; e-mail, purduenews@purdue.edu
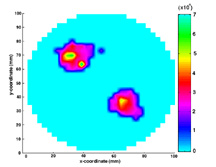
NOTE TO JOURNALISTS: A color computer image of the simulated reconstruction of diseased tissue and a copy of the scientific paper are available from Purdue News Service, (765) 494-2096. Ask for the photo called Sevick/Fluorescence Imaging or download here.
Abstract
Imaging of fluorescent yield and lifetime from multiply scattered light re-emitted from tissues and other random media
D.Y. Paithankar, A.U. Chen, E.M. Sevick-Muraca, School of Chemical Engineering, Purdue University; B.W. Pogue, Wellman Laboratories of Photomedicine, Massachusetts General Hospital, Harvard Medical School; M.S. Patterson, Hamilton Regional Cancer Center, Medical Physics Dept., Ontario, Canada.
The feasibility of employing fluorescent contrast agents to perform optical imaging in tissues and other scattering media has been examined through computational studies. Fluorescence lifetime and yield can give crucial information about local metabolite concentration or environmental conditions within tissues. This information can be employed towards disease detection, diagnosis, and treatment if non-invasively quantitated from re-emitted optical signals. However, the problem of inverse image reconstruction of fluorescence yield and lifetime is complicated due to the highly scattering nature of the tissue. In this work, a light propagation model employing the diffusion equation is used to account for the scattering of both the excitation and fluorescent light. Simulated measurements of frequency-domain parameters of fluorescent modulated AC intensity and phase-lag are used as inputs to an inverse image reconstruction algorithm which employs the diffusion model to relate frequency-domain measurements resulting from a modulated input at the phantom periphery. In the inverse image reconstruction algorithm, we employ a Newton-Raphson technique combined with Marquardt algorithm to converge upon the fluorescent properties within the medium. The successful reconstruction of both the fluorescence yield and lifetime in the case of heterogeneous fluorophore distribution within a scattering medium has been demonstrated without a priori information or without the necessity of obtaining "absence" images.